For more information on the Medicare accreditation requirement for entities billing the technical component for advanced diagnostic imaging (CT, MRI, PET/Nuclear Medicine) effective January 1, 2012, read my post here.
—————————————————————————————–
Medicare Learning Network (MLN) just released MM6912, effective August 2, 2010: Mailing To All Individual Practitioners, Medical Groups and Clinics and Independent Diagnostic Testing Facilities (IDTF) Who Are Billing or Have Billed For The Technical Component of Advanced Diagnostic Imaging Services
What exactly is an IDTF?
Some suppliers that perform diagnostic tests, other than clinical laboratory or pathology tests, are required to enroll with Medicare as an Independent Diagnostic Testing Facility (IDTF). Not all suppliers that perform these diagnostic tests are required to enroll as an IDTF. Generally, entities can bill for the technical component of the diagnostic tests without an IDTF enrollment if it has the following characteristics:
- A physician practice that is owned, directly or indirectly, by one or more physicians or by a hospital
- A facility that primarily bills for physician services and not for diagnostic tests
- A facility that furnishes diagnostic tests primarily to patients whose medical conditions are being treated or managed on an ongoing basis by one or more physicians in the practice
- The diagnostic tests are performed and interpreted at the same location where the practice physicians also treat patients for their medical conditions
- If a substantial portion of the facility’s business involves the performance of diagnostic tests, the diagnostic testing services may be a sufficient separate business to require enrollment as an IDTF. In that case, the physician or physician group practice can continue to be enrolled as a physician or physician group practice but are also required to enroll as an IDTF. The physician or group can bill for professional fees and the diagnostic tests they perform on their patients using their billing number. Therefore, the practice must bill as an IDTF for diagnostic tests furnished to Medicare beneficiaries who are not regular patients of the physician or group practice.
Who will receive a mailing?
Enrolled physicians, non-physician practitioners, including single and multi- specialty clinics, and IDTFs who have billed the Medicare program for the technical component of advanced diagnostic testing services within the preceding six month period and who continue to have Medicare billing privileges with Medicare contractors (carriers and Part A/B Medicare Administrative Contractors (A/B MACs)) are affected.
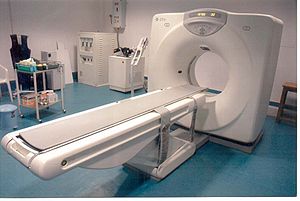
Image via Wikipedia
If you have billed the Medicare program for the technical component of advanced diagnostic testing services within the preceding six month period and continue to have Medicare billing privileges with Medicare contractors, you will receive a letter from your Medicare contractor advising you of the need to become accredited by January 1, 2012, in order to continue to provide these services and bill Medicare.
When more than one physician or non-physician practitioner is operating within a group, such as a single specialty or multispecialty clinic, only the group will receive the letter, not each of the individual physicians or non-physician practitioners working for the group.
What will the mailing say?
You must be accredited by one of the three Centers for Medicare & Medicaid
Services (CMS) approved national accreditation organizations by January 1, 2012,
in order to be eligible to continue to furnish the technical component of advanced
diagnostic testing services to Medicare beneficiaries and submit claims for those
services to your Medicare contractor.
Your contractor will be mailing the letter quarterly beginning with July 2010 through July 2011. If necessary, follow the instructions in the letter to become accredited by January 1, 2012, in order to continue billing for the technical component of advance diagnostic imaging services. Make sure that your office staffs are aware of these new accreditation requirements and begin the accreditation process as soon as possible to protect your Medicare billing rights for these services.
Why do IDTFs have to become accredited now?
Section 135(a) of the Medicare Improvements for Patients and Providers Act of
2008 (MIPPA) amended section 1834(e) of the Social Security Act and required
the Secretary, Health and Human Services, to designate organizations to accredit
suppliers, including but not limited to physicians, non-physician practitioners and
Independent Diagnostic Testing Facilities, that furnish the technical component
(TC) of advanced diagnostic imaging services.
What qualifies as an advanced diagnostic imaging procedure?
MIPPA specifically defines advanced diagnostic imaging procedures as including:
Ӣ Diagnostic magnetic resonance imaging (MRI),
Ӣ Computed tomography (CT), and
Ӣ Nuclear medicine imaging, such as positron emission tomography (PET).
MIPPA expressly excludes from the accreditation requirement x-ray, ultrasound,
and fluoroscopy procedures. The law also excludes from the CMS accreditation
requirement diagnostic and screening mammography, which are subject to quality oversight by the Food and Drug Administration under the Mammography Quality Standards Act.
How long does it take to become accredited?
Since CMS expects that it may take as much as nine months from the time you initiate the accreditation process to completion, you should begin the accreditation process for advanced diagnostic imaging services as soon as possible, but not later than March 2011.
Who are the accrediting organizations?
CMS approved three national accreditation organizations — the American College
of Radiology, the Intersocietal Accreditation Commission, and The Joint
Commission — to provide accreditation services for suppliers of the TC of advanced diagnostic imaging procedures. The accreditation will apply only to
the suppliers of the images themselves, and not to the physician interpreting
the image. All accreditation organizations have quality standards that address the safety of the equipment as well as the safety of the patients and staff.
If you have questions, contact your Medicare carrier and/or A/B MAC at
their toll-free number, which may be found here (zip file.)

Image via Wikipedia
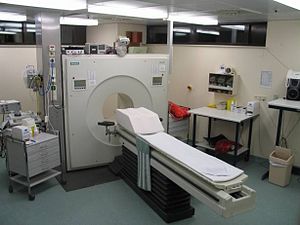
Image via Wikipedia
The letter will look like this:
[DATE]
[Supplier Name and Address]
Dear Physician/Non-Physician Practitioner/IDTF owner:
In accordance with Section 135(a) of the Medicare Improvements for Patients and Providers Act of 2008 (MIPPA), suppliers, including but not limited to physicians, non-physician practitioners and Independent Diagnostic Testing Facilities that furnish the technical component (TC) of advanced diagnostic imaging services must be accredited by January 1, 2012 in order to continue to furnish these services to Medicare beneficiaries.
Our records indicate that you have furnished advanced diagnostic imaging procedures such as diagnostic magnetic resonance imaging (MRI), computed tomography (CT), and nuclear medicine imaging such as positron emission tomography (PET) within the last six months. If you are not accredited by one of the organizations shown below by January 1, 2012, you will not be eligible to bill the Medicare program for advanced diagnostic imaging services. This letter requests that you take the necessary action to become accredited by the January 1, 2012 deadline. Since we expect it can take up to nine months from the time you initiate the accreditation process to completion, we urge you to begin the accreditation process for advanced diagnostic imaging services as soon as possible.
MIPPA expressly excludes from the accreditation requirement x-ray, ultrasound, and fluoroscopy procedures. The law also excludes from the CMS accreditation requirement diagnostic and screening mammography which are already subject to quality oversight by the Food and Drug Administration under the Mammography Quality Standards Act.
The Centers for Medicare & Medicaid Services (CMS) approved three national accreditation organizations ”“ the American College of Radiology, the Intersocietal Accreditation Commission, and The Joint Commission – to provide accreditation services for suppliers of the TC of advanced diagnostic imaging procedures. The accreditation will apply only to the suppliers of the images themselves, and not to the physician interpreting the image. All accreditation organizations have quality standards that address the safety of the equipment as well as the safety of the patients and staff. The accrediting organization that issues your accreditation will notify Medicare once your accreditation is complete and approved.
To obtain additional information about the accreditation process, please contact the accreditation organizations shown below.
Image by Jon Olav via Flickr
American College of Radiology (ACR)
1891 Preston White Drive
Reston, VA 20191-4326
1-800-770-0145
Intersocietal Accreditation Commission (IAC)
6021 University Boulevard, Suite 500
Ellicott City, MD 21043
1-800-838-2110
The Joint Commission (TJC)
Ambulatory Care Accreditation Program
One Renaissance Boulevard
Oakbrook Terrace, IL 60181
1-630-792-5286
If you have questions about this letter, contact [carrier or A/B MAC phone number/contact person].
Sincerely,
[Name of carrier or A/B MAC]
******************************************************************
Supplier Billed Advanced Medical Imaging CPT codes for Section 135 (a) of the MIPPA to Receive Accreditation Requirement Notification Letter
70336 70540 71250 72125 73200 74150
70450 70542 71260 72126 73201 74160
70460 70543 71270 72127 73202 74170
70470 70544 71275 72128 73206 74175
70480 70545 71550 72129 73218 74181
70481 70546 71551 72130 73219 74182
70482 70547 71552 72131 73220 74183
70486 70548 71555 72132 73221 74185
70487 70549 72133 73222
70488 70551 72141 73223
70490 70552 72142 73225
70491 70553 72146 73700
70492 70554 72147 73701
70496 70555 72148 73702
70498 70557 72149 73706
70558 72156 73718
70559 72157 7371972158 73720
72159 73721
72191 73722
72192 73723
72193 73725
72194
72195
72196
72197
72198
72200
75557 76360 77011 78000 78811
75559 76376 77012 78001 78812
75561 76377 77021 78003 78813
75563 76380 77058 78006 78814
76390 77059 78007 78815
76497 77078 78010 78816
76498 77079 78011 78891
78015
78016
78018
78020
78070
78075
78099


